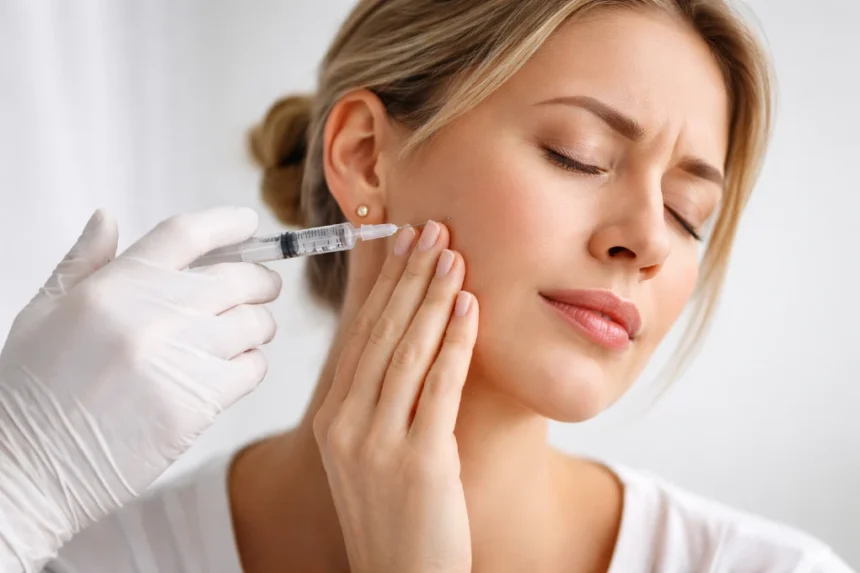
If you have ever woken up with a sore jaw, tension around your temples, or that dull ache that seems to travel from your face to your neck, you have probably wondered whether there is a treatment that actually works. That is why so many people are searching for Botox for TMJ. It is often discussed as a way to ease jaw pain, reduce clenching, and calm overworked facial muscles when more basic treatments have not done enough.
- What TMJ actually means
- How Botox for TMJ works
- Does Botox for TMJ really help jaw pain and clenching?
- What the procedure is like
- How long Botox for TMJ takes to work
- Potential benefits of Botox for TMJ
- Risks and side effects to know
- Is Botox for TMJ FDA approved?
- Botox for TMJ vs mouth guards and conservative treatment
- Who may be a good candidate for Botox for TMJ
- What results feel like in real life
- Practical tips if you are considering Botox for TMJ
- Final thoughts on whether Botox for TMJ is worth it
The interest makes sense. Temporomandibular disorders, often called TMD, affect the jaw joint and the muscles around it, and the condition is far more common than many people realize. The National Institute of Dental and Craniofacial Research estimates that about 5% to 10% of people in the United States have some form of TMD, with women affected more often than men. <a href=”https://www.nidcr.nih.gov/grants-funding/funded-research/research-investments-advances/temporomandibular-disorders” rel=”nofollow”>NIDCR</a>
So, does Botox for TMJ really help? In many cases, it can help reduce muscle-related jaw pain, facial tension, and clenching, especially when symptoms are driven by overactive chewing muscles. But it is not a magic fix, and it is not the right answer for every type of TMJ problem. The real value lies in knowing who may benefit, what the treatment can and cannot do, and how it compares with other options.
What TMJ actually means
People often say “TMJ” when they are talking about jaw pain, but TMJ is technically the temporomandibular joint itself. The broader condition is called TMD, or temporomandibular disorder. According to NIDCR, TMD includes more than 30 conditions that can affect the jaw joint, chewing muscles, and surrounding tissues. <a href=”https://www.nidcr.nih.gov/health-info/tmd” rel=”nofollow”>NIDCR TMD overview</a>
Common symptoms include:
- Jaw pain or tenderness
- Clicking, popping, or grinding in the jaw
- Tightness when opening the mouth
- Headaches or temple pain
- Facial soreness
- Ear-area discomfort
- Teeth grinding or clenching, also called bruxism
- Neck and shoulder tension
This matters because Botox for TMJ tends to work best for muscle-driven symptoms, not every possible jaw disorder. If the main problem is joint damage, arthritis, or a displaced disc inside the joint, Botox may not address the root cause.
How Botox for TMJ works
Botox for TMJ uses botulinum toxin type A, a purified neurotoxin that temporarily reduces muscle activity. When injected into overactive muscles, usually the masseter and sometimes the temporalis, it blocks the nerve signals that tell those muscles to contract so forcefully.
In simpler terms, it helps calm the constant overworking of the jaw muscles.
That can be useful for people who:
- Clench during the day without realizing it
- Grind their teeth at night
- Have painful, enlarged masseter muscles
- Feel constant muscle tension in the jaw and temples
- Have myofascial jaw pain that has not improved enough with conservative care
Because the muscles relax, Botox for TMJ may reduce the force of clenching, ease pressure-related pain, and give irritated tissues a chance to settle down.
Does Botox for TMJ really help jaw pain and clenching?
The honest answer is yes, it can help, but the evidence is mixed and the results are not universal.
A 2024 systematic review in PLOS One found that the current evidence does not support definitive conclusions that botulinum toxin is clearly superior to placebo or other treatments across all TMD cases. At the same time, several studies and reviews suggest it may help selected patients, especially those with muscular TMD, bruxism-related pain, and persistent myofascial symptoms. <a href=”https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0300157″ rel=”nofollow”>PLOS One systematic review</a> <a href=”https://www.jofph.com/articles/10.11607/ofph.3023″ rel=”nofollow”>Journal of Oral & Facial Pain and Headache review</a>
That tells us something important. Botox for TMJ is not a universal first-line cure. It is better viewed as a targeted option for the right patient.
Where it may help most
Botox for TMJ may be most useful when symptoms are caused largely by muscle overuse, such as:
- Chronic jaw clenching
- Teeth grinding with sore masseter muscles
- Temple headaches linked to jaw tension
- Pain when chewing because the jaw muscles stay tight
- Muscle hypertrophy, where the jawline looks wider because the masseters are overdeveloped
Where it may help less
It may be less effective when the main issue is:
- A structural joint problem
- Advanced joint degeneration
- Inflammatory arthritis
- A major bite problem that needs dental correction
- Stress-driven habits that return unless behavioral factors are addressed
So yes, Botox for TMJ can help some people quite a bit, but it works best when the diagnosis is accurate.
What the procedure is like
Getting Botox for TMJ is usually a quick outpatient treatment. A dentist, oral surgeon, facial pain specialist, or other trained medical injector examines the jaw, identifies the muscles involved, and places a series of small injections into the target muscles.
Most sessions take about 10 to 20 minutes.
A typical appointment includes:
- Review of symptoms and jaw function
- Palpation of the masseter and temporalis muscles
- Marking of injection points
- Small injections with a fine needle
- Return to normal activity soon afterward
The discomfort is often described as brief and manageable. Many people go right back to work the same day.
How long Botox for TMJ takes to work
This is one of the most common questions, and it is a fair one.
Botox for TMJ usually does not work instantly. Some people notice changes in a few days, but it often takes 1 to 2 weeks to feel the full effect. The muscle-relaxing action develops gradually.
For many patients:
- Early changes may begin within 3 to 7 days
- More noticeable relief often appears by 10 to 14 days
- Results may last around 3 to 4 months
- Repeat sessions may be needed to maintain benefits
That timeline is one reason Botox for TMJ is often considered part of a broader treatment plan rather than a one-time solution.
Potential benefits of Botox for TMJ
When it is used in the right setting, Botox for TMJ may offer several practical benefits.
1. Less jaw muscle tension
This is often the biggest win. When the masseter muscles are constantly working overtime, they become sore, tight, and tender. Botox can reduce that constant tension.
2. Reduced clenching force
For people who clench hard, especially during sleep or stressful periods, Botox for TMJ may reduce the power of those contractions. That can mean less strain on the jaw muscles and surrounding tissues.
3. Fewer tension headaches
Some patients notice improvement in temple pressure or headache symptoms when jaw muscle tension drops.
4. Better comfort during chewing
Pain when chewing can improve when the muscles are not in a constant state of overload.
5. Jawline slimming in some cases
This is not the primary medical goal, but it can happen. If enlarged masseter muscles are part of the issue, Botox for TMJ may gradually soften the appearance of a square jawline.
Risks and side effects to know
No medical treatment is risk-free, and Botox for TMJ is no exception.
Possible side effects include:
- Injection-site soreness
- Mild bruising
- Temporary chewing fatigue
- Smile asymmetry if product spreads to nearby muscles
- Changes in bite force
- Weakness when eating hard or chewy foods
There are also longer-term concerns that clinicians consider, especially with repeated treatment. Some reviews note concerns about possible muscle atrophy and, in certain settings, effects on bone or joint loading over time if dosing is too aggressive or repeated without careful follow-up. <a href=”https://www.cda-amc.ca/botulinum-toxin-temporomandibular-disorders-review-clinical-effectiveness-cost-effectiveness-and” rel=”nofollow”>CADTH review</a> <a href=”https://www.sciencedirect.com/science/article/pii/S0266435624004832″ rel=”nofollow”>British Journal of Oral and Maxillofacial Surgery review</a>
This is why Botox for TMJ should be done by someone who understands both facial anatomy and TMJ disorders, not just cosmetic injection technique.
Is Botox for TMJ FDA approved?
This is another important point. Botox for TMJ is commonly used, but it is generally considered an off-label treatment for TMD. Off-label use is legal and common in medicine, but it means the treatment is being used in a way that does not have a specific FDA approval for this exact indication.
That does not automatically mean it is unsafe. It means patients should understand that the evidence is still evolving and that clinical judgment matters.
Botox for TMJ vs mouth guards and conservative treatment
For many people, Botox for TMJ should not be the first thing they try.
Conservative care often comes first, including:
- Soft diet during flare-ups
- Heat or ice
- Jaw stretching and physical therapy
- Stress management
- Better sleep habits
- Avoiding gum chewing
- Night guards or splints when appropriate
- Anti-inflammatory medication if recommended by a clinician
The NHS notes that bruxism and teeth grinding are often linked with stress, sleep factors, or dental issues, and management may involve mouth guards and habit-focused treatment. <a href=”https://www.nhs.uk/symptoms/teeth-grinding/” rel=”nofollow”>NHS bruxism information</a>
Here is a quick comparison:
| Treatment | Best for | Pros | Limits |
|---|---|---|---|
| Mouth guard | Grinding, tooth protection | Noninvasive, common | Does not relax muscles directly |
| Physical therapy | Muscle imbalance, joint stiffness | Improves function | Needs consistency |
| Self-care and habit changes | Mild to moderate symptoms | Low cost, helpful early | May not be enough alone |
| Botox for TMJ | Muscle-driven pain and clenching | Can reduce tension and force | Temporary, costlier, not for every TMJ type |
This is why a careful diagnosis matters more than hype.
Who may be a good candidate for Botox for TMJ
A person may be a reasonable candidate for Botox for TMJ if:
- Jaw pain appears to be muscular rather than purely joint-based
- Clenching or bruxism is a major issue
- Conservative treatment has not provided enough relief
- The masseter or temporalis muscles are clearly overactive
- They understand the treatment is temporary and may require repeat sessions
A person may not be the best candidate if:
- The pain source is unclear
- They have a significant underlying joint disorder needing other treatment
- They are pregnant or breastfeeding, depending on clinician advice
- They have a neuromuscular condition that makes Botox unsuitable
- They want a permanent cure from a temporary treatment
What results feel like in real life
People often expect dramatic change right away, but Botox for TMJ usually works in a more subtle, functional way.
You may notice:
- You are not clenching as hard
- Your face feels less tight by late afternoon
- Morning jaw soreness fades
- Chewing feels easier
- Headache frequency drops
- Your jaw feels less “worked out” all the time
That kind of improvement can be meaningful, especially for someone who has been stuck in a cycle of pain, stress, and clenching for months.
Practical tips if you are considering Botox for TMJ
If you are thinking seriously about Botox for TMJ, these steps can make a big difference:
Get the diagnosis right
Make sure a qualified clinician confirms whether your pain is muscular, joint-related, or mixed.
Ask about all treatment options
Botox should be compared with splints, physical therapy, habit retraining, and medical management, not viewed in isolation.
Start with realistic expectations
Botox for TMJ may reduce symptoms, not erase every cause of jaw pain.
Track your symptoms
Before treatment, note your pain level, clenching frequency, headaches, and chewing discomfort. This makes it easier to judge whether it helped.
Choose an experienced provider
The best injector for Botox for TMJ is someone who treats jaw disorders regularly and understands functional anatomy.
Final thoughts on whether Botox for TMJ is worth it
So, does Botox for TMJ really help jaw pain and clenching? For the right person, yes, it can. It may reduce muscle tension, soften clenching force, and improve day-to-day comfort when overactive jaw muscles are driving the problem. But it is not a one-size-fits-all fix, and it should not replace a proper diagnosis.
The smartest approach is to treat Botox for TMJ as one possible tool within a larger care plan. If your symptoms are mostly muscular and you have already tried more conservative options without enough relief, it may be worth discussing with a qualified provider. If the problem is more structural or joint-based, other treatments may make more sense.
Understanding the bigger picture of the jaw joint is what helps patients make better decisions. And when you make the decision based on diagnosis rather than trend, you are far more likely to get a result that actually feels worth it.